Hallux rigidus is the medical term used to describe a painful, stiff big toe. The name means stiff (rigidus) great toe (hallux). The joint affected is the first metatarsophalangeal joint (MTPJ).
Like arthritis elsewhere in the body, it often develops spontaneously with no apparent reason. Your genetics may play an influencing role in this. Other causes of hallux rigidus include rheumatoid arthritis, gout, and trauma.
Normal cartilage allows the metatarsal (long bones of the foot) and proximal phalanx (first small bone of the toe) to glide against one another. When this cartilage thins and disappears, this movement becomes painful. The body can sense this process and often attempts to grow extra bone around the joint, named osteophytes, which make the joint stiffer. You can often feel osteophytes on the dorsal (top) and medial (inner) aspects of the joint as firm bony lumps.
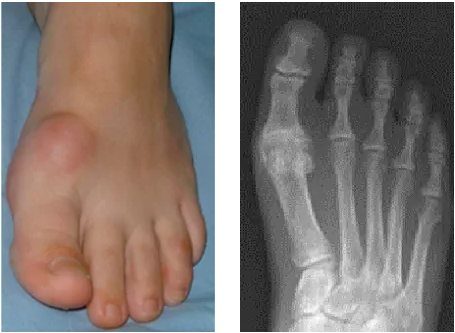
symptoms
Patients may complain of pain, stiffness, or both. Pain in some patients is only when they bend their big toe beyond a certain angle, and this is important in determining options for treatment. This may make it difficult to run, play sport or wear high heels. Pain that is constant or occurs with movement in any position of the toe may indicate severe arthritis. Pain only at the maximum extent of movement may indicate less severe arthritis, or a region of localised arthritis.
non-operative treatment
The treatment of hallux rigidus includes an array of methods to relieve pain and restore function before considering surgery.
- Shoe modification
- High heels put significant pressure on the head of the first metatarsal. Avoiding high heels can considerably improve pain.
- Rocker bottom shoes have a specially designed rounded sole. This reduces the need to bend your toes maximally back at the point just before you lift your foot off the ground during walking, which reduces the pressure on this joint and reduces symptoms.
- High quality rocker bottom shoes can be expensive however are often highly effective.
- Orthotics can be fashioned to stiffen the sole of a shoe (extended shank)1 and relieve some of the pressure on your big toe during walking.
- Pain medication
- A combination of regular paracetamol and intermittent non-steroidal anti-inflammatories (NSAIDs Nurofen, Celebrex, Mobic).
- If you have been diagnosed with neuropathic (nerve) pain in addition to arthritis, nerve-specific medication such as gabapentin or pregabalin may be beneficial.
- Opiate and similar pain medication (Oxycodone, Endone, Oxycontin, Tramadol, Palexia) are useful in the short term but rarely effective in managing long term pain.
- All medications carry risks and side effects, and you should discuss these with your local doctor, sports doctor, or surgeon before commencing.
operative treatment
It is important to thoroughly review a patient’s symptoms, perform a comprehensive physical examination and thoroughly inspect imaging to determine the need for, and most appropriate, operative treatment. There is often a mismatch between the severity of symptoms and the changes apparent on an X-Ray1. Therefore, the profile of pain and other symptoms is more important in determining whether to proceed with surgery than the appearance of the X-Rays.
Cheilectomy
The least invasive option is a dorsal cheilectomy. This procedure involves shaving away the prominent bony osteophytes, particularly from the top of the joint. This procedure can improve the range of movement at the joint and relieve pain that occurs due to bony impingement when the toe is bent up. A cheilectomy can be performed either through a small incision or using key-hole techniques. The bone is removed with a saw or a burr.
Moberg Osteotomy
The Moberg osteotomy is a procedure to re-orient the proximal phalanx2. The goal of this procedure is to allow the toe to point up more, at the expense of pointing towards the floor. It does not change the overall size of the arc of movement but shifts the arc to allow the toe to point up. It involves removing a small wedge of bone, and then fixation with a small screw.
A Moberg osteotomy would often be performed in conjunction with a cheilectomy to both gain upward movement of the toe and reduce the pain with maximal movement.
Fusion
Arthritis of the great toe can be very effectively treated by fusing the joint. This is performed using a plate, screws, or a combination of both. Once solidly fused the joint does not move at all, which is highly effective at eliminating pain. This comes at a sacrifice in movement and is an important consideration. Patients who undergo a fusion will not be able to wear high heeled shoes. Running is possible with a great toe fusion, but longer distance running may be difficult. Normal daily activities and walking are minimally affected.
Joint Replacement
A total joint replacement (total arthroplasty), or a partial replacement (hemiarthroplasty) can be performed for hallux rigidus. This surgery is like a fusion, except instead of plates and screws to hold the joint immobile, implants are placed on the ends of the metatarsal head only (hemiarthroplasty) or both the metatarsal and proximal phalanx (total arthroplasty). This surgery is not commonly performed as the longer-term outcomes have not been as positive when compared with fusion3.
Cartiva
Cartiva is a relatively new product designed for treatment of hallux rigidus while also preserving joint motion. It is made of a hydrogel material and acts in a similar fashion to a joint replacement. The implant is inserted onto the surface of the head of the first metatarsal and runs smoothly over the cartilage on the proximal phalanx. It has the advantage of preserving movement, however any significant arthritis on the proximal phalanx side of the joint risks ongoing pain. In patients who do not want a fusion, this is a useful alternative.
contact
This fact sheet is a brief overview of Hallux Rigidus (Big Toe Arthritis), produced by our Foot and Ankle Surgeon Dr Thomas Fisher. To make an appointment or enquiry with Dr Fisher or a member of our foot and ankle team, contact 08 8362 7788 or email ortho@sportsmed.com.au.
References
1. Kunnasegaran R, Thevendran G. Hallux Rigidus Nonoperative Treatment and Orthotics. Foot Ankle Clin. 2015;20(3):401–12.
2. Warganich T, Harris T. Moberg Osteotomy for Hallux Rigidus. Foot Ankle Clin. 2015;20(3):433–50.
3. Deland JT, Williams BR. Surgical Management of Hallux Rigidus. J Am Acad Orthop Sur. 2012;20(6):347–58.



