Osteoarthritis (OA) occurs when the cartilage that cushions the ends of bones in your joints gradually deteriorates. Cartilage is a firm, slippery tissue that enables nearly frictionless joint motion. Eventually, as the cartilage wears down, it effects the underlying bone and causes pain. Osteoarthritis has often been referred to as a wear and tear disease but besides the breakdown of cartilage, OA affects the entire joint. It causes changes in the bone and deterioration of the connective tissues that hold the joint together and attach muscle to bone, as well as inflammation of the joint lining.
Osteoarthritis is the most common lifestyle disease in people older than 65. Like all chronic conditions, exercise is a critical component of its management.
There are many studies that show exercise is effective for osteoarthritis, but most are small in participant numbers and have very varied exercise protocols.
We know pain and function have positive outcomes with exercise in those who are supervised and known to be compliant with the programs – that’s the critical part. We also know that if you do nothing other than lose 10-15% of your body weight that your pain and function also improve, so a combination of these things is logically particularly effective.
founders
Professor Ewa Roos and Dr Soren Skou of the University of Southern Denmark developed the exercise program, carried it out on almost 10,000 participants, and published the results in 2017. Among the findings were increased physical activity at 3 and 12 months, reduced sick leave at 12 months, and reduced pain medication at 3 months.
who
Professor Ewa Roos and Dr Soren Skou of the University of Southern Denmark developed the exercise It’s important to know the program is for the full spectrum of knee and hip OA, as long as you’re reasonably mobile. It’s not designed to manage rheumatological joint arthritis.
what
The program includes 12 hours of supervised exercise, 2 hours of education, as well as outcome measures. It’s done ideally over 6 weeks, and costs $518. This is all explained at the initial review. It should be noted that we run this program not only at Stepney, but at Morphett Vale as well.
We register those willing to do the supervised class training within our gym, although if this is impractical such as due to travel issues, we will still try to teach you some of the exercises 1:1 and review periodically as required.
We also do a face-to-face follow up at 3 months after registration, which is after they’ve had a chance to continue the program at home or at their gym. At this review we re-do the outcome measures.
aim
The program’s aim is to build your neuromuscular strength capacity, and by doing this, we get to push your tolerance to whatever daily life throws at you.
As strength capacity improves, it allows you to target a more active general lifestyle in volume and / or intensity.
In addition to a reduced risk of flare ups during general activity, there is also a risk reduction in other chronic conditions that benefit from exercise such as cardiac, diabetes, and mental health issues.
pain
One of the key strategies in ensuring low flare up risk and the appropriate level of prescription of the program, is pain monitoring.
The term ‘Safe and Acceptable Level’ of 0-5/10 pain score during and after the sessions, seems to resonate well, and this is part of the education.
The combination of any pain levels along with our observation of the quality of their exercise drives the specific level of exercise prescription we choose, and again helps minimise flare ups along the way to better ensure consistent gains.
our experience
Over a 3 year period of running this program, the graph in diagram 1 shows the average reported pain scores before and after the exercise classes from class 1 through to 12.
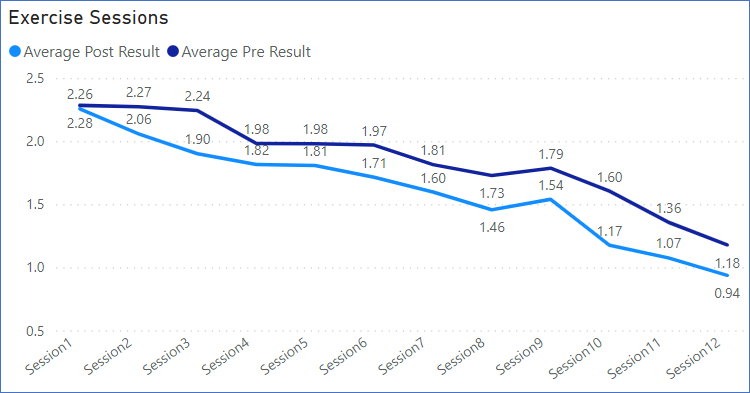
We are very confident that the participants are tolerating the program. Not only were the pain scores lower after the class, but they also trended downwards as the course went on.
The supervision component here is critical as it allows us to help the participants pitch the exercise at the right level, understand the exercise, improve technique, and very importantly reduce their fears associated with exercise.
By the end of the program most patients are very capable in the exercises, and how best to self-prescribe their individual intensity and volume to match their capacity.
This achievement is hugely important in the whole program’s success. Once you graduate, you then have the best chance at remaining compliant and continuing to do it unsupervised at home or in their gym x 2/week.
results at sportsmed
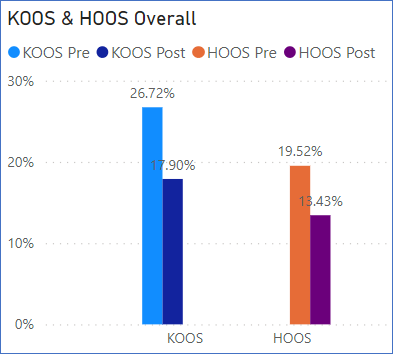
The KOOS (Knee Osteoarthritis Outcome Score) and HOOS (Hip Osteoarthritis Outcome Score) are both patient-reported outcome scores.
Across all our participants, these scores had improved by over 30% at the 3 month follow up.
The Activities of Daily Living section improved by almost 50%, the Pain score by 35%, and Quality of Life by 30%.
take home message
GLA:D is a set 12 session program, ideally over 6 weeks. It is supervised, individually tailored, and is well tolerated.
Importantly, 12 sessions of training appears to be enough to make you very capable within the program, which follows onto a better chance for ongoing compliance either at home or the gym.
Outcome scores improved by over 30% at 3 months follow up, and this is consistent with the original large Danish study published in 2017.
contact
The GLA:D Osteoarthritis Program us available at our Stepney Healthcare Hub, as well as our Morphett Vale Branch. To make an appointment, enquiry or check the latest class times, contact 08 8362 8122 or email physio@sportsmed.com.au.



